
Previous
Does Liver Cancer Cause Green Stool?

Next
The Best Liver Detoxes and Liver Cleanses Out There
Does Liver Disease Treat Men and Women Equally?
Discover if gender can have anything to do with the manifestation of liver disease. If so, do men or women have it worse?
Gender equality is typically viewed as a political movement regarding equal opportunities and compensation regardless of sexual category. However, did you know that liver disease may not treat men and women equally?
The physiological differences between males and females lead to a few liver-related gender disparities.
Emerging as a valuable field of research, gender-based medicine is a new concept investigating how disease manifests differently in men and women – and could warrant different evaluation, monitoring, and treatment.
The Liver Performs the Same Critical Functions for Men and Women
Regardless of gender, the liver, your body’s largest solid organ, performs the same key functions for both men and women:
- Filters toxins out of the bloodstream
- Makes bile, a fluid that aids in the digestion of food – especially fats
- Stores extra glucose as glycogen for when the body needs it for energy
- Produces blood-clotting factors
- Makes amino acids – the building blocks for proteins – including amino acids used to fight infection
- Processes and stores iron for red blood cell production
- Manufactures hormones, cholesterol, and other chemicals needed to transport fat
- Converts waste products into urea for excretion in the urine
- Metabolizes chemicals and medications
About Liver Injury and Disease
Liver disease is a broad term describing many different problems that interfere with your liver’s ability to function, and can cause significant damage to your liver’s ability to fulfill its responsibilities. However, your liver is unique in its ability to easily replace damaged cells.
But, if the source of injury is persistent, the liver cell damage can outpace liver cell regeneration and your liver will not be able to reverse this damage. This imbalance leads to fibrosis, areas of dead liver cells that create scars and, if the damage grows, it can lead to death.
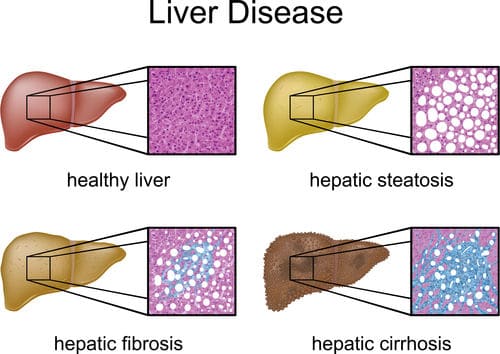
Some of the more common types of liver disease include:
- Infectious hepatitis – Liver cell inflammation that is caused by a virus, such as Hepatitis A, Hepatitis B, Hepatitis C and Hepatitis D.
- Autoimmune hepatitis – When the body’s immune system, which ordinarily attacks viruses, bacteria and other pathogens, instead targets the liver.
- Hepatocellular carcinoma (HCC) – Primary malignant tumor of the liver.
- Non-alcoholic liver disease (NAFLD) – Describes the accumulation of fat within the liver that is not caused by drinking alcohol. If NAFLD progresses, it can cause liver inflammation that gradually hampers liver function.
- Alcoholic liver disease (ALD) – Occurring after years of heavy drinking, ALD damages the liver, leads to a buildup of fat in the liver, inflammation, and fibrosis. If unchecked, ALD typically leads to cirrhosis.
- Primary biliary cholangitis – A chronic liver disease caused by progressive destruction of the bile ducts.
- Hepatic encephalopathy (HE) – HE is a complication of advanced liver disease where toxins accumulate in the brain.
- Acetaminophen-induced acute liver injury – Patients unintentionally take took much acetaminophen and/or other analgesics.
Gender Differences and Liver Disease
Examining differences in liver disease between men and women is an emerging area of research. Though, clinicians have recognized gender variances in the epidemiology, progression and treatment strategies of certain liver diseases for a while.
The findings appear to be unfavorable for women:

- According to Seth Levin, DO, a gastroenterologist with the OhioHealth Physician Group, “Women are more prone to certain types of liver disease, such as autoimmune hepatitis, primary biliary cholangitis and toxin mediated liver injury, which includes alcohol-induced liver injury. They are also more likely to present with acute liver failure and to develop benign liver lesions.”
- Levin says that although men are more likely to abuse alcohol than women, women are more susceptible to its toxicity on the liver – regardless of how much is imbibed. In addition, women who develop ALD are likely to see it progress more rapidly then men with ALD.
- As published in a 2017 Thai study of over 34,000 participants in F1000 Research, NAFLD is most prevalent in women who are 56-60 years old. The authors concluded that post-menopausal women should be the target for interventions or further investigation for NAFLD.
- As published in the June 2018 edition of Clinical Gastroenterology and Hepatology, American researchers analyzed gender differences in acetaminophen-induced liver toxicity. They found that acetaminophen-induced acute liver injury and acute liver failure were more common among women. In addition, their data suggested that women have greater critical care needs than men, and increased risk for severe hepatic encephalopathy (HE), which could be due in part to increased use of sedatives. The researchers believe future studies should investigate sex differences in acetaminophen metabolism and hepatotoxicity, particularly among users of opioids.
On the other hand, researchers have uncovered several exceptions to females suffering more from liver disease:
- In general, men are 2-fold more likely to die from chronic liver disease and cirrhosis than are women.
- In a prospective study of 490,000 men and women in the United States followed for 9 years, the relative risk of death from cirrhosis or alcoholism was equal in both sexes for those drinking 2 to 3 drinks per day but was increased in men who drank 4 or more drinks per day.
- While the majority of benign liver tumors are more common in women, malignant tumors are more common in men.
- Hepatocellular carcinoma (HCC) is the most common primary malignant tumor of the liver and affects men 3 to 4 times more frequently than women.
- Women clear acute Hepatitis C virus (HCV) infection at a higher rate than men.
Conclusion
While the field of gender-based hepatology is in its infancy, scholars surmise the differences in liver disease expression are likely due to sex hormones, physical body size/mass, and metabolic variations by gender.
Ultimately, learning about different presentations and outcomes of liver disease in men and women can influence testing, predictions, and treatment based on gender – an approach that could eventually reduce the overall burden of liver disease.
http://www.gastroenterologyandhepatology.net/archives/october-2013/liver-disease-in-women-influence-of-gender-on-epidemiology-natural-history-and-patient-outcomes/, Liver Disease in Women: Influence of Gender on Epidemiology, Natural History, and Patient Outcomes, J. Guy, MD and M. Peters, MD, Retrieved July 8, 2018, Millenium Medical Publishing, 2018.
https://www.healthyway.com/content/liver-disease-symptoms-cant-be-ignored-but-do-you-know-whos-at-risk/, Liver Disease Symptoms Can’t Be Ignored: But Do You Know Who’s At Risk?, Jeanne Sager, Retrieved July 8, 2018, Multiply Media, LLC, 2018.
https://www.jwatch.org/na45741/2017/12/20/gender-disparities-acetaminophen-induced-acute-liver, Gender Disparities in Acetaminophen-Induced Acute Liver Failure, Atif Zaman, MD, MPH, Retrieved July 8, 2018, Clinical Gastroenterology and Hepatology, June 2018.
https://www.medicinenet.com/liver_disease/article.htm#what_is_liver_disease, What is Liver Disease?, Retrieved July 8, 2018, MedicineNet, Inc., 2018.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5645706/, Gender differences in the prevalence of nonalcoholic fatty liver disease in the Northeast of Thailand: A population-based cross-sectional study, B. Thinkhamrop, et al, Retrieved July 8, 2018, F1000 Research, October 2017.
https://www.ncbi.nlm.nih.gov/pubmed/28336373, Gender differences in liver disease and the drug-dose gender gap, Buzzetti, E, et al, Retrieved July 8, 2018, Pharmacological Research, June 2017.






